Blogs
Tips, Facts, And The
Latest In Dentistry

What Is the Step-by-Step Procedure for Getting Full Mouth Dental Implants?
Posted in Dental Implants
Posted on March 2, 2026 by thedigitalsmile

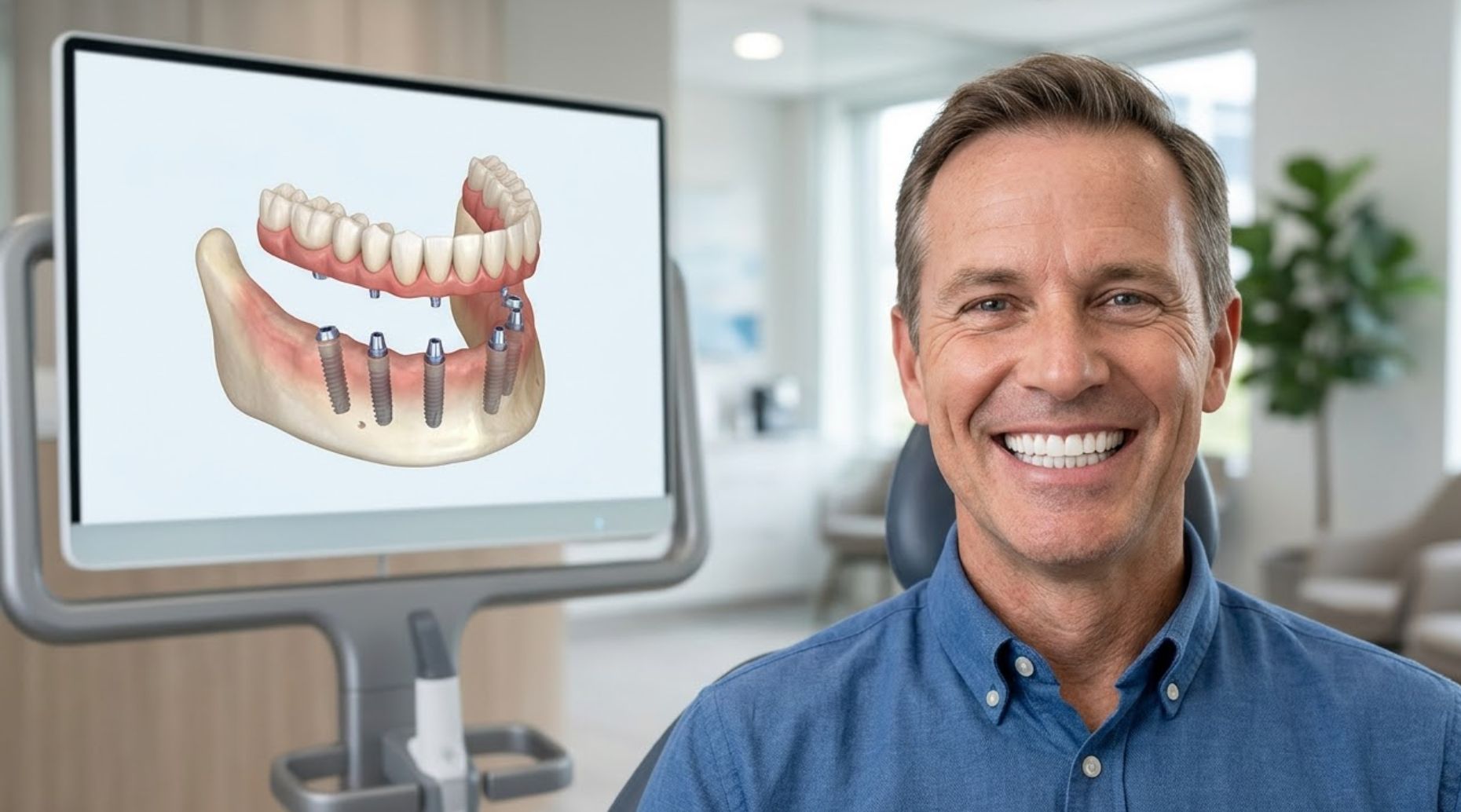
Full mouth dental implants are a restorative option for patients seeking to recover oral function and smile aesthetics. This guide describes each stage of the process, from initial consultation through final restoration. Many patients present with tooth loss, caries, or periodontal disease that impair chewing, speech, and quality of life. Full mouth implants provide improved stability and appearance compared with conventional removable dentures. The following sections explain consultation, individualized planning, surgical steps, healing, and post-treatment care so patients understand what to expect.
A clinical case example is provided to demonstrate the combined surgical and prosthetic protocols used in full mouth implant rehabilitation.
Full Mouth Implant Rehabilitation: Surgical & Prosthetic Protocol
A 60-year-old female patient presented with multiple missing teeth and advanced periodontal disease. Preoperative clinical and radiographic examination revealed that all her remaining teeth were periodontally compromised with Grade III mobility [Table/Fig-1]. She had no history of allergies or any other medical illness. The treatment plan was extraction of all her teeth and its replacement with maxillary and mandibular removable complete dentures. The patient was very keen on having a fixed prosthesis in order to avoid wearing the conventional removable dentures. A total extraction of all her teeth was performed along with alveolectomy and ridge reduction to obtain an optimum prosthetic platform. After initial healing period of 2 weeks, the impressions were taken and an interim denture was made. The transition of interim denture to Procera Implant Bridge (PIB) took around 40 days to complete stereolithographic surgical template, guided surgery and prosthetic rehabilitation.
Implant–supported full mouth rehabilitation: A guided surgical and prosthetic protocol, N Sakkir, 2016
Initial Consultation and Assessment
The initial consultation establishes candidacy for full mouth implants. The dental team records medical and dental history, reviews previous notes, and obtains diagnostic imaging to assess bone volume and oral pathology. These data inform risk assessment and help determine whether adjunctive procedures, such as bone grafting or extractions, are required. A clear assessment permits a tailored treatment plan.
Personalized Treatment Plan
A bespoke treatment plan is developed from the assessment and imaging results. The plan sets out proposed procedures, expected functional and aesthetic outcomes, and an estimated timeline. The dental team discusses options and potential constraints with the patient so the final plan aligns with clinical needs and patient preferences.
Implant Surgery
Implant surgery involves the precise placement of endosseous implants into the jawbone to serve as anchors for the prosthesis. Appropriate anaesthesia is provided to ensure patient comfort. The surgical team follows the planned implant positions, often guided by surgical templates or computer navigation, to optimise biomechanics and long-term prognosis. Post-operative instructions are issued to support recovery.
Healing and Osseointegration
Healing after implant placement enables osseointegration, the biological fusion of implant and bone. This phase typically spans several weeks and is critical for implant stability. Patients attend follow-up reviews to monitor soft tissue healing and integration. Compliance with postoperative instructions supports predictable outcomes.
Abutment Placement
Following satisfactory osseointegration, abutments are connected to the implants. These components provide the interface between the implant and the prosthetic teeth. The procedure is performed under local anaesthesia and is generally straightforward. Proper abutment selection and placement are essential for the accuracy and longevity of the final restoration.
Final Restoration
The final prosthesis is fitted to the abutments and adjusted to achieve the desired aesthetics, occlusion, and comfort. The clinical team verifies fit and function and makes necessary refinements. Long-term maintenance requirements, including routine examinations and hygiene protocols, are reviewed to preserve implant health.
Speranza Dental Implant Centers specialises in advanced implant care, focusing on full mouth dental implants and immediate load protocols to deliver consistent, high-quality treatment throughout the care pathway.
Follow-Up Care
Structured follow-up is necessary to safeguard implant longevity. Regular clinical reviews assess peri-implant tissues, occlusion, and prosthesis integrity. Patients receive instruction on oral hygiene measures specific to implants to reduce infection risk. Early detection of issues improves long-term prognosis.
What Is the Initial Consultation and Candidacy Assessment for Full Mouth Dental Implants?
The initial consultation includes a detailed medical and dental history, clinical examination, and diagnostic imaging. These steps identify factors that influence candidacy, such as bone availability, periodontal status, and systemic health considerations that may require modification of the plan.
Which Criteria Determine Patient Eligibility for Full Arch Dental Implants?
Eligibility for full-arch implants depends on several factors, including sufficient bone volume, controlled periodontal and endodontic conditions, and a medical history that does not contraindicate surgery. Each factor is evaluated to determine the appropriate treatment pathway.
- Bone Density Requirements: Sufficient bone density is necessary to support the implants.
- Overall Oral Health: Patients must have healthy gums and no active dental infections.
- Medical History Considerations: Certain medical conditions may affect candidacy, requiring careful evaluation.
How Does Speranza Dental Implant Centers Personalize Treatment Plans?
Speranza Dental Implant Centers designs individualised plans using comprehensive clinical assessment and advanced imaging. This process enables precise surgical and prosthetic planning and ensures patients understand their options and expected outcomes.
How Is Imaging and Treatment Planning Conducted for Full Mouth Implant Surgery?
Imaging and planning for full mouth implant surgery follow a staged process that collects clinical data, constructs anatomical models, and develops a surgical strategy to place implants in optimal positions for function and longevity.
- Initial Consultation: The dental team gathers comprehensive health information.
- Diagnostic Imaging: Advanced imaging techniques, such as Cone Beam Computed Tomography (CBCT), are used to create detailed 3D models of the jaw.
- Surgical Planning: The data collected is used to develop a precise surgical plan that optimizes implant placement.
What Advanced Imaging Technologies Are Used in Implant Planning?
Advanced imaging, notably Cone Beam Computed Tomography (CBCT), provides three-dimensional assessment of the jaws and local anatomy. These data support implant position planning and help avoid vital structures. Computer-guided workflows improve placement accuracy and clinical predictability.
The importance of advanced imaging in this process is underscored by research highlighting the benefits of technologies like Cone Beam Computed Tomography (CBCT) for precise preoperative planning.
CBCT Imaging for Preoperative Dental Implant Planning
Orofacial diagnostic imaging has grown dramatically in recent years. As the use of endosseous implants has revolutionized oral rehabilitation, a specialized technique has become available for the preoperative planning of oral implant placement: cone beam computed tomography (CT). This imaging technology provides 3D and cross-sectional views of the jaws. It is obvious that this hardware is not in the same class as CT machines in cost, size, weight, complexity, and radiation dose. It is thus considered to be the examination of choice when making a risk–benefit assessment. The present review deals with imaging modalities available for preoperative planning purposes with a specific focus on the use of the cone beam CT and software for planning of oral implant surgery.
State-of-the-art on cone beam CT imaging for preoperative planning of implant placement, ME Guerrero, 2006
How Does Treatment Planning Optimize Implant Placement and Outcomes?
Rigorous treatment planning uses clinical and radiographic data to select implant sites that maximise bone contact and prosthetic support. Precise planning reduces intraoperative risk and improves the probability of successful osseointegration and long-term function.
What Are the Surgical Steps Involved in Full Mouth Dental Implant Placement?
The core surgical steps include patient assessment, diagnostic imaging, and the surgical placement of implants according to the predetermined plan. Each step is executed to maintain clinical accuracy and procedural safety.
- Initial Consultation: Gathering patient information and conducting assessments.
- Diagnostic Imaging: Utilizing advanced imaging to plan the surgery.
- Surgical Procedure: Carefully placing the implants into the jawbone according to the surgical plan.
How Is the Surgical Procedure Executed Step-by-Step?
The surgical sequence begins with patient preparation and anaesthesia, followed by guided implant placement and concludes with clear post-operative care instructions to support healing and recovery.
- Preparation: The patient is prepared for surgery, and anesthesia is administered.
- Implant Placement: The dental team places the implants into the jawbone with precision.
- Post-Operative Care: Instructions are provided to ensure proper healing and recovery.
What Are the Differences Between Immediate Load and Traditional Implant Protocols?
Immediate load protocols permit placement of provisional prosthetics at the time of surgery, while traditional protocols delay restoration until after an integration period. Immediate loading can reduce time without functional teeth but must be selected based on clinical stability and case-specific factors. Long-term outcomes depend on case selection and surgical execution.
- Treatment Time: Immediate load implants allow for the placement of temporary prosthetics on the same day as surgery, while traditional protocols require a healing period before restoration.
- Patient Comfort: Immediate load options can enhance patient comfort by providing a functional solution sooner.
- Long-Term Outcomes: Both approaches have unique benefits, and the choice depends on individual patient needs and circumstances.
What Is the Recovery Timeline and Aftercare Following Full Mouth Implant Surgery?
Recovery typically extends over several weeks. Early healing involves transient swelling and discomfort managed with prescribed medication. The osseointegration phase follows and requires monitoring. Scheduled follow-up visits allow the team to assess healing and address any concerns.
- Initial Healing: The first few days involve swelling and discomfort, managed with prescribed medications.
- Osseointegration: This critical phase lasts several weeks, during which the implants integrate with the jawbone.
- Follow-Up Care: Regular check-ups are essential to monitor healing and address any concerns.
What Is the Typical Healing Process and Duration?
Healing progresses through immediate postoperative recovery, a period of osseointegration, and subsequent prosthetic adjustments. Osseointegration commonly requires 8–12 weeks. Regular clinical reviews ensure appropriate healing and permit timely adjustments.
- Swelling and Discomfort: Initial swelling and discomfort are common but manageable with care.
- Osseointegration: This phase, lasting 8-12 weeks, is crucial for the stability of the implants.
- Follow-Up Visits: Regular follow-up visits ensure proper healing and allow for adjustments as needed.
Which Postoperative Care Practices Enhance Patient Outcomes?
Effective postoperative care includes meticulous oral hygiene, adherence to dietary recommendations, and attendance at scheduled follow-up appointments. These measures reduce infection risk and support optimal healing.
- Maintaining Oral Hygiene: Proper oral hygiene is essential for preventing infections.
- Dietary Recommendations: Soft foods are recommended during the initial healing phase.
- Regular Follow-Up Appointments: Consistent check-ups help monitor implant health and address any issues promptly.
How Is the Final Restoration Completed and What Follow-Up Care Is Required?
Final restoration involves abutment connection, fitting and adjustment of the prosthetic teeth, and confirmation of function and aesthetics. Ongoing recall visits are required to maintain peri-implant health and prosthesis performance.
- Abutment Attachment: Abutments are attached to the implants to support the prosthetic teeth.
- Fitting of Prosthetic Teeth: The dental team ensures a proper fit and makes necessary adjustments.
- Follow-Up Care: Ongoing follow-up care is essential for maintaining implant health and function.
What Are the Steps for Attaching the Final Prosthesis?
Attaching the final prosthesis includes secure abutment connection, precise seating of the prosthetic, and final occlusal and aesthetic adjustments to ensure patient comfort and function.
- Abutment Attachment: Securely attaching the abutments to the implants.
- Final Adjustments: Making adjustments to ensure comfort and aesthetics.
- Patient Comfort: Ensuring the patient is satisfied with the final result.
How Does Ongoing Maintenance Support Long-Term Implant Success?
Long-term success depends on daily oral hygiene, routine dental examinations, and proactive management of peri-implant tissues. These practices minimise complications and extend prosthesis lifespan.
- Oral Hygiene Practices: Regular brushing and flossing help maintain implant health.
- Regular Dental Check-Ups: Consistent visits to the dental office allow for monitoring and early detection of issues.
- Preventing Complications: Proactive care helps prevent complications that could jeopardize the implants.
What Patient Experiences and Success Stories Illustrate the Benefits of Full Mouth Implants?
Patient reports commonly describe improved masticatory function, greater confidence, and enhanced overall quality of life following full mouth implant treatment. Such outcomes underscore the value of experienced clinicians and careful planning.
How Have Immediate Load Implants Improved Patient Quality of Life?
Immediate load implants provide provisional function and appearance on the day of surgery for appropriately selected patients. This approach can reduce the interval without functional teeth and support faster return to normal activities when clinically indicated.
Frequently Asked Questions
What are the potential risks and complications associated with full mouth dental implants?
Full mouth implant treatment is generally predictable but carries risks such as surgical-site infection, sensory nerve disturbance, sinus complications, and implant failure related to inadequate osseointegration. Patients with uncontrolled systemic conditions, for example diabetes or certain immune disorders, may have increased risk and require careful assessment and management during planning.
How long do full mouth dental implants typically last?
Full mouth dental implants are intended as a long-term solution and commonly last 10 to 15 years or longer with appropriate care. Longevity depends on oral hygiene, regular professional maintenance, and factors such as smoking and general health. Ongoing monitoring and care improve the likelihood of durable results.
What is the cost range for full mouth dental implants?
The cost varies by case complexity, materials, and geographic location. Typical treatment costs for a complete set of full mouth implants range from $20,000 to $50,000. A detailed assessment with the provider will yield a personalised estimate and information on financing options.
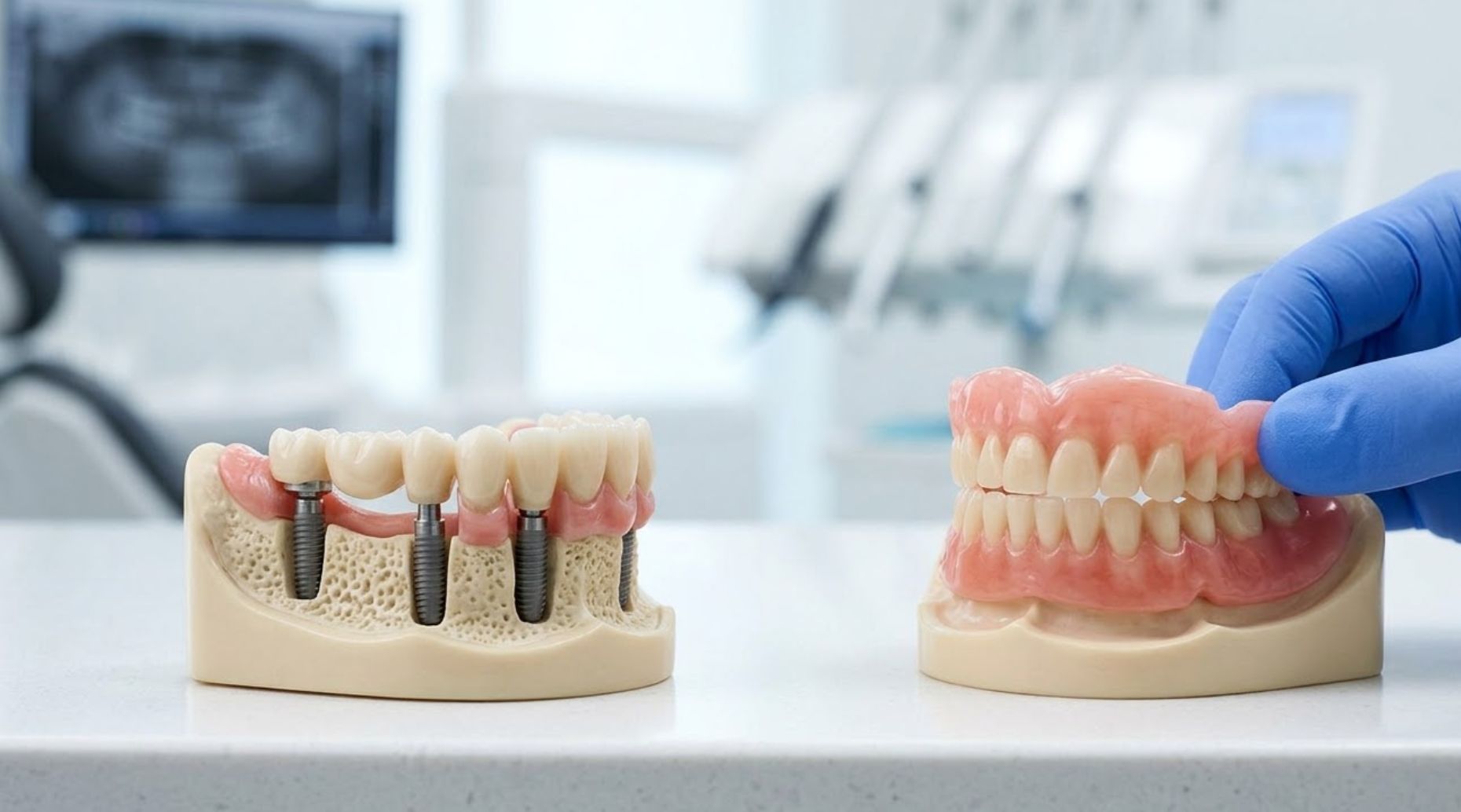
Are there alternatives to full mouth dental implants?
Alternatives include conventional complete dentures, partial dentures, and fixed or removable bridges. Each option has advantages and limitations regarding invasiveness, stability, function, and cost. A clinician can advise on the most suitable solution based on clinical findings and patient priorities.
What should I expect during the recovery process after implant surgery?
Recovery commonly takes several weeks. Early symptoms include swelling and discomfort that are typically controlled with prescribed analgesics. The osseointegration period, during which implants fuse with bone, generally lasts 8–12 weeks. Follow-up appointments are scheduled to monitor healing and manage any issues.
How can I maintain my full mouth dental implants for long-term success?
Maintenance requires daily brushing and interdental cleaning with non-abrasive products, avoidance of tobacco, a balanced diet, and regular professional reviews. Prompt attention to signs of peri-implant inflammation or prosthetic wear supports long-term performance.
Conclusion
Full mouth dental implants restore function and aesthetics and can materially improve patient quality of life when planned and executed by an experienced team. Understanding the treatment stages—from assessment through final prosthesis and maintenance—helps patients make informed decisions. Contact our team to discuss personalised options and next steps for care.