Blogs
Tips, Facts, And The
Latest In Dentistry

What Are the Potential Risks and Complications of Full Mouth Dental Implants?
Posted in Dental Implants
Posted on March 14, 2026 by thedigitalsmile
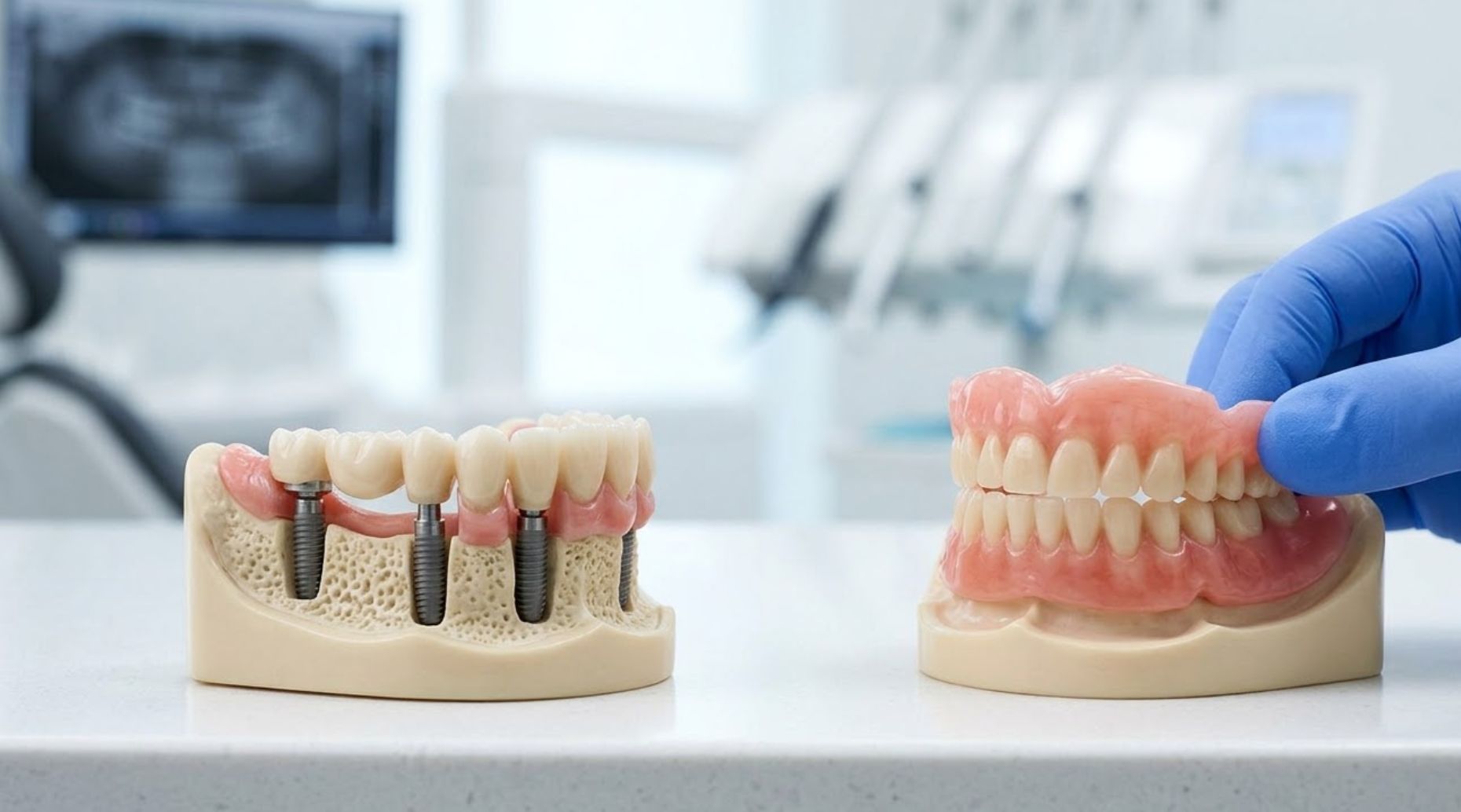
Full mouth dental implants provide a durable solution for complete tooth replacement. Like all surgical interventions, they carry potential risks and complications that patients must understand. This article reviews the principal risks—such as infection, implant failure, and complications related to bone grafting—and explains preventive measures, post-operative care, and the potential financial impact of complications.
What Are the Most Common Risks Associated with Full Mouth Dental Implants?
When evaluating full mouth dental implants, patients should be aware of the most common risks. These risks can influence procedural success and overall oral health.
- Infection Risk: Infection can occur at the implant site, leading to complications that may require additional treatment.
- Nerve Irritation: The placement of implants can sometimes irritate nearby nerves, causing discomfort or numbness.
- Sinus Issues: In some cases, implants placed in the upper jaw can protrude into the sinus cavity, leading to sinus problems.
Speranza Dental Implant Centers, located in Sarasota, FL, specializes in full mouth dental implants and offers comprehensive consultations to review these risks in detail.
How Does Infection Impact Full Mouth Dental Implant Success?
Infection is a major threat to implant success. Bacterial contamination of the surgical site can produce peri-implantitis—an inflammatory process with progressive bone loss around the implant—which may lead to implant failure if not treated promptly.
Strict pre- and post-operative oral hygiene reduces infection risk. Scheduled follow-up visits allow the dental team to monitor healing and identify early signs of infection.
What Are the Causes and Signs of Implant Failure?
Implant failure may arise from multiple factors; early recognition enables timely management. Common causes of implant failure include:
- Excessive Stress on Implants: Overloading the implants with excessive force can lead to failure.
- Poor Oral Hygiene: Neglecting oral care can result in infections that compromise the implant.
- Signs of Instability: Patients may notice looseness or movement of the implant, indicating potential failure.
Recognising these signs and maintaining rigorous oral hygiene substantially improves implant longevity.
Which Complications Arise from Bone Grafting in Full Mouth Implants?
Bone grafting is frequently required when alveolar bone volume is insufficient to support implants. The procedure carries specific complications, including:
- Infection at Graft Site: Just like with implants, the graft site can become infected, complicating the healing process.
- Nerve Injury: There is a risk of nerve damage during the grafting procedure, which can lead to numbness or pain.
- Bone Resorption: In some cases, the grafted bone may not integrate properly, leading to resorption and loss of the graft.
Clear communication with the dental team about these risks helps patients prepare and make informed decisions regarding grafting and implant timing.
What Are the Potential Side Effects of Bone Graft Procedures?
Bone graft procedures produce predictable side effects that warrant patient consideration. These can include:
- Swelling and Discomfort: Patients often experience swelling and discomfort at the graft site, which can be managed with medication.
- Delayed Healing: Some individuals may experience longer healing times, which can postpone the implant placement.
- General Risks of Dental Implant Surgery: As with any surgical procedure, there are inherent risks, including bleeding and adverse reactions to anesthesia.
Selecting an experienced surgical team and adhering to clinical guidance reduces these risks and supports favorable outcomes.
How Can Bone Graft Risks Be Minimized?
To reduce the risks associated with bone grafting, patients can take several proactive steps:
- Comprehensive Assessment: A thorough evaluation by a dental professional can determine the need for grafting and the best approach.
- Choosing the Right Provider: Selecting an experienced surgeon can significantly impact the success of the procedure.
- Post-Procedure Care: Following all post-operative instructions, including medication and dietary recommendations, is crucial for healing.
Following these precautions improves the probability of successful graft integration and subsequent implant placement.
What Are the Neurological Risks and Numbness Associated with Full Mouth Implants?
Neurological complications, chiefly nerve injury, are a recognised risk with full mouth implant placement. Injury may produce temporary or permanent numbness in the lips, tongue, or chin.
Accurate knowledge of mandibular and maxillary nerve anatomy is essential for risk reduction. Patients should review anatomical considerations and surgical plans with their clinician prior to surgery.
How Does Nerve Damage Occur During Implant Surgery?
Nerve damage during implant surgery can occur due to several factors, including:
- Improper Implant Placement: Incorrect positioning of the implant can inadvertently affect nearby nerves.
- Poor Bone Quality: Insufficient bone density can complicate the placement and increase the risk of nerve injury.
Understanding these technical factors underscores the importance of selecting a clinician with appropriate implant and grafting experience.
What Symptoms Indicate Nerve Injury After Implant Placement?
Patients should be vigilant for symptoms that may indicate nerve injury following implant placement, such as:
- Numbness in Lip or Tongue: A loss of sensation in these areas can signal nerve damage.
- Tingling Sensations: Unusual tingling or burning sensations may also indicate nerve involvement.
Any of these findings warrants immediate evaluation by the treating dentist to determine the need for diagnostic assessment or intervention.
How Can Patients Prevent and Manage Complications After Full Mouth Dental Implants?
Preventing and managing complications requires active patient participation and clinician oversight. Key strategies include:
- Follow Post-Operative Instructions: Adhering to the care guidelines provided by your dental team is crucial for recovery.
- Maintain Good Oral Hygiene: Regular brushing and flossing can help prevent infections.
- Regular Follow-Up Appointments: Keeping scheduled appointments allows for monitoring of the healing process and early detection of any issues.
Patient adherence to postoperative instructions and routine monitoring materially reduces complication rates.
What Are the Best Practices for Post-Operative Care?
Effective post-operative care is vital for the success of full mouth dental implants. Best practices include:
- Pain and Swelling Management: Utilizing prescribed medications can help manage discomfort and reduce swelling.
- Dietary Recommendations: Following a soft food diet initially can prevent stress on the implants.
- Recognizing Complications: Being aware of signs of complications, such as persistent pain or unusual swelling, is essential for timely intervention.
These measures support healing, reduce complications, and contribute to long-term implant stability.
When Should Patients Contact Their Dentist About Possible Complications?
Patients should be proactive in monitoring their recovery and should contact their dentist if they experience:
- Persistent Pain: Ongoing discomfort that does not improve may indicate a problem.
- Unusual Swelling: Significant swelling that worsens could be a sign of infection.
- Changes in Gum Tissue: Any alterations in the appearance or health of the gums should be evaluated.
Prompt communication with the dental team enables early diagnosis and treatment, limiting progression of complications.
What Are the Cost Implications of Complications in Full Mouth Dental Implant Procedures?
Complications arising from full mouth dental implants can lead to significant cost implications. Additional procedures may be required to address issues such as infections or implant failures, which can increase overall treatment costs.
Awareness of potential costs allows patients to plan financially and discuss risk mitigation and contingency strategies with their provider.
How Do Complications Affect Overall Treatment Costs?
The presence of complications can substantially affect the overall costs associated with full mouth dental implants. Factors include:
- Need for Extra Surgeries: Complications may necessitate additional surgical interventions, increasing expenses.
- Extended Recovery Times: Prolonged healing periods can lead to additional follow-up visits and associated costs.
Anticipating these scenarios helps patients evaluate the financial implications of implant therapy.
Are There Insurance or Financing Options for Managing Complication Costs?
Patients concerned about the financial implications of complications should explore various insurance and financing options available to them. These may include:
- Insurance Coverage Details: Some insurance plans may cover a portion of the costs associated with complications.
- Payment Plans: Many dental practices offer financing options to help manage out-of-pocket expenses.
- Health Savings Accounts: Utilizing HSA funds can provide tax advantages for medical expenses related to dental care.
Reviewing coverage details and payment plans with the practice and insurers can clarify financial responsibilities and support treatment planning.
Frequently Asked Questions
What is the recovery timeline after full mouth dental implant surgery?
Recovery timelines vary by patient. Soft-tissue healing typically occurs within 1 to 2 weeks, while osseointegration—the process of bone integrating with the implant—generally requires 3 to 6 months. Regular follow-up appointments are essential to verify successful integration and guide timing for final prosthetic restoration.
What lifestyle changes should I consider after getting full mouth implants?
After full mouth implant placement, patients should adopt measures that support healing: follow a soft-food diet during initial recovery, maintain meticulous oral hygiene using recommended tools and techniques, and avoid tobacco and excessive alcohol to reduce complication risk.
How can I manage pain and discomfort after the procedure?
Post-operative pain is managed with prescribed analgesics and, when appropriate, short courses of anti-inflammatory medication. Application of ice to the facial area can reduce swelling. Patients should follow the dentist’s postoperative instructions, including medication dosing and dietary guidance, to minimize discomfort.
What should I do if I notice signs of infection after surgery?
If you notice signs of infection after your full mouth dental implant surgery, such as increased swelling, persistent pain, or discharge from the surgical site, it is crucial to contact your dentist immediately. Early intervention typically involves antibiotic therapy and local management to protect implant integrity.
Are there specific foods I should avoid after getting implants?
During initial healing, avoid hard, crunchy, or sticky foods that place excessive load on implants. Also limit very hot or spicy items that may irritate the surgical site. Opt for soft foods such as yogurt, mashed potatoes, and smoothies to facilitate comfort and recovery.
How often should I schedule follow-up appointments after my implants are placed?
Follow-up visits are critical during the initial healing phase; patients commonly attend appointments every few weeks for the first 3 to 6 months. Once osseointegration is confirmed, routine dental examinations every 6 to 12 months are recommended to monitor implant health.
Conclusion
Understanding the risks of full mouth dental implants—such as infection, nerve injury, and bone graft complications—enables patients to make informed decisions. Regular consultations with a qualified implant team, adherence to postoperative protocols, and timely communication about concerns all contribute to successful outcomes. For personalized guidance and to discuss treatment options, contact us to schedule a consultation.